Pityrosporum folliculitis, also known as Malassezia folliculitis is a condition that causes breakouts on your skin.
It happens when the yeast which naturally lives on your skin, gets into your hair follicles and manifests itself through causing breakouts in areas with a lot of sebaceous activity.
This can be the T-zone, shoulders, back, and chest.
While typical acne breakouts can be blamed on hormones, clogged pores, and overgrowth of the bad bacteria living on the skin, malassezia folliculitis distinguishes itself from these.
It has absolutely nothing to do with hormones and clogged pores because it is an overgrowth of yeast that causes the breakouts.
Malassezia folliculitis can be challenging to recognize and is often misdiagnosed for common acne vulgaris.
This misdiagnose can very often lead to the suggestion of wrong treatment options that may potentially aggravate the condition instead of improving it.
So how can we recognize the difference between acne vulgaris and Malassezia folliculitis?

What Is Malassezia Folliculitis?
Malassezia folliculitis is an infection of hair follicles caused by lipophilic malassezia yeasts.
It is a species of fungi that is a part of the skin’s microbiome which is essentially the first line of defense against disease, infection, and pathogen attack.
Often referred to as our acid mantle, the microbiome has a pH of 4.5 – 5.5 and maintains the ideal environment to prevent pathogen attacks and promote the growth of healthy bacteria on the skin.
Changes in pH, low levels of hydration, and harsh environmental factors can all take effect on the bacteria living on your skin.
This essentially leads to the conclusion that “one bad bacterium too many” can cause massive flare-ups, sensitivity, blemishes, and…you’ve guessed it?
Fungal infections.
Malassezia folliculitis is a polymorphic, lipophilic microorganism, which means that this little *says something really bad* thrives in the presence of sebum which is our natural oil produced by the sebaceous glands to keep our skin naturally moisturized.
Different Species of Malassezia Folliculitis
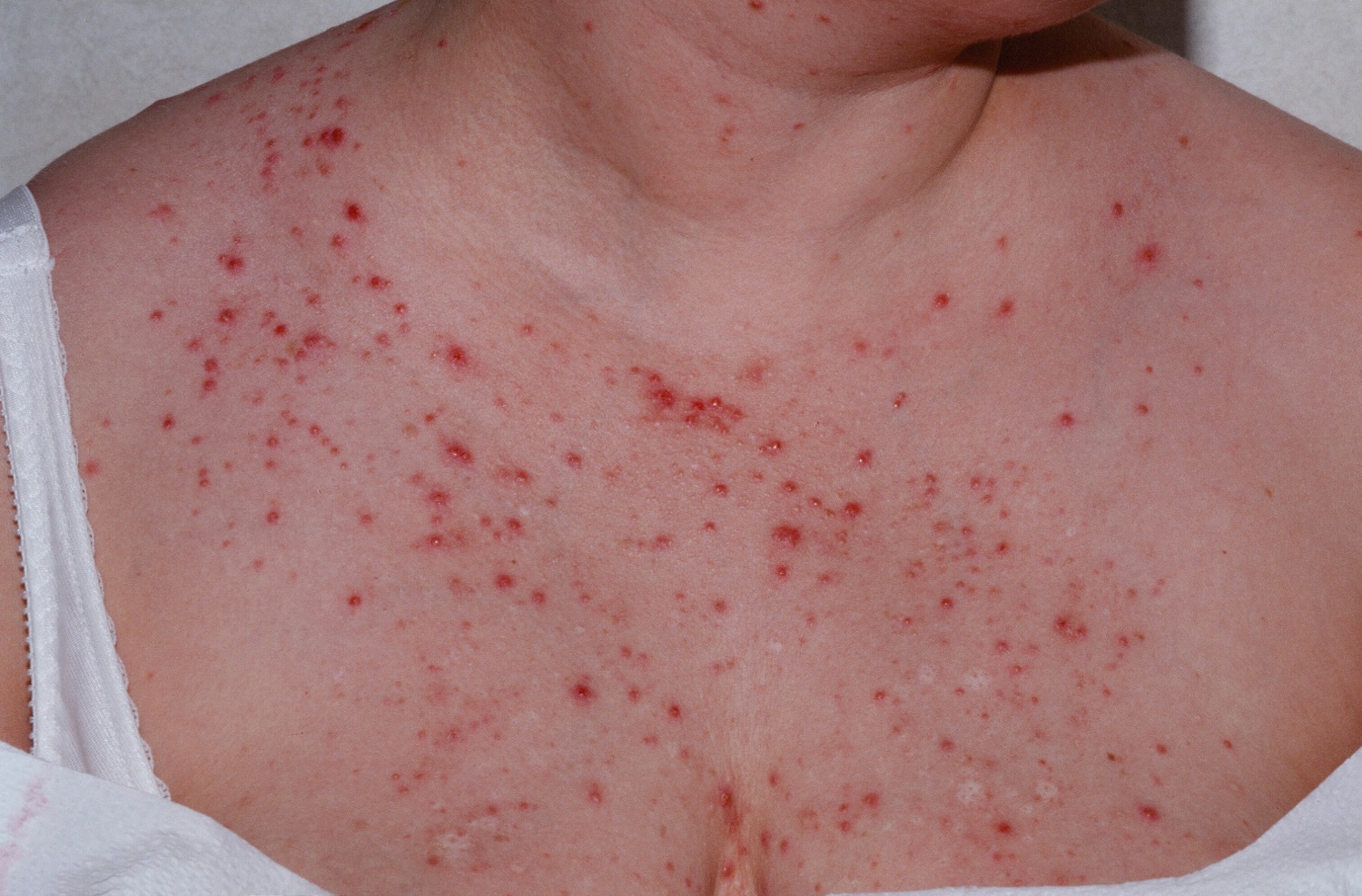
There are multiple malassezia species that have been isolated from human and animal skin and some of them include:
- M. furfur
- M. globosa
- M. sympodialis
- M. restricta
Malassezia folliculitis is most commonly associated with Malassezia furfur and Malassezia globosa but the pathogenic yeast plays a role in many other skin conditions, such as:
- dandruff
- seborrheic dermatitis
- psoriasis
- eczema
- tinea (pityriasis) versicolor – fungal infection on the skin.
What Causes Malassezia Folliculitis?
Malassezia infections are mostly endogenous, which means that they are produced from the inside of the skin and originate from colonized skin.
It is caused by an overgrowth of yeast that gets into the hair follicles, uses the sebum in the follicle as food and fuel to thrive, and causes breakouts to erupt on the skin’s surface.
Malassezia is incapable of synthesizing its own fatty acids, and it needs sebum to build its own mid-length and long-chain fatty acids in order to thrive.
Or in simple terms: Malassezia gets into the hair follicles of our skin and considers the place to be a grocery store.
Antibiotics, birth control pills, hormonal changes, and medicine used to stabilize hormones are also very likely to develop this condition, as they disrupt the natural balance of bacteria on and in your body.
Why Is It Important To Recognize Malassezia Folliculitis?
The reason it’s important to distinguish Malassezia folliculitis is that it can very easily be misdiagnosed with common acne breakouts.
Depending on the severity of the breakouts you may be prescribed strong antibiotics such as Accutane in order to treat the condition effectively.
While Accutane is known to have some serious side effects, this treatment will not improve malassezia folliculitis, but on the contrary, the yeast is able to find a way to thrive beside it, making the condition even worse.
You can recognize if you have malassezia folliculitis by following the pattern of the growth and placement of the occurring breakout.
Areas that are more active in sebum production such as the T-zone is the ideal placement for the yeast to thrive, so this area is most commonly affected, unlike common bacterial or hormonal acne breakouts that typically occur on the cheeks and jawline.
If you are suspecting that you have malassezia folliculitis rather than acne vulgaris, see a dermatologist and ask to be specifically tested for this condition before arriving at your appointment.
The doctor will need to scratch your skin gently in the area where you have the symptoms to get a cell sample.
This will then be evaluated under a microscope and tested to see if it’s pitryosporum folliculitis (the actual condition).
How to Treat Malassezia Folliculitis Successfully?

There are several treatments your doctor can prescribe for this condition.
The first and most important principle in treating this condition is to eliminate predisposing factors.
If you are currently taking oral antibiotics and suspecting that you have pityrosporum folliculitis, discontinuing the antibiotics may result in mild improvement.
Additionally, your doctor may prescribe taking an oral antifungal drug called Itraconazole for seven days and following it up with monthly maintenance.
Itraconazole has shown to have some of the best medical outcomes after several searches have been done.
Since many people (myself included) have both acne and pityrosporum folliculitis due to malassezia, a prescription cocktail including both steroid and topical anti-acne cream may be prescribed.
Other topical remedies that you can use to treat pityosporum folliculitis at home can include selenium sulfide shampoo, purchased from the pharmacy, or Econazole cream to kill the overgrowth of yeast on your skin.
Lastly, if your condition can be considered mild, you can try applying diluted tea tree oil to the area up to twice a day.
I have personally found swimming in the sea extremely helpful for my condition, so bathing in a solution of sea salt may also help to dry out the skin and treat the yeast overgrowth.
Malassezia (Pityrosporum) folliculitis, unfortunately, cannot be prevented.
But there are steps you can take to reduce the risks of future breakouts.
Pay close attention and care for areas on the skin that are prone to oil buildups. Additionally, washing with an antifungal soap and shampoo may help make your skin less prone to yeast overgrowth.
Observe any changes in the problematic areas and visit a doctor if you think it’s necessary.

My name is Simone and I am a certified skin specialist. I created this website to teach my readers how to take great care of their skin and I also like to occasionally share my honest opinions on skincare products I’ve tried. You can learn more about me here.

Thank you Simone – great run down of this condition, and also for pointing out the different types of ‘acne’ on your face (that was very helpful for me). I too am very angry about the treatment my daughter has received due to misdiagnosis and flippant and TOTALLY incorrect care, and subsequent harm, she has received from doctors and dermatologist for over a decade. And to think, THEY are supposed to be the experts :'(
Thank you for your kind words and I am so sorry that happened but thankfully, you’ve managed to discover and address the issue. Thing is that Malassezia Folliculitis is a difficult condition to recognize, especially when you consider the fact that it’s not as common as typical acne is. I hope all is well now!