Post-inflammatory hyperpigmentation (PIH) is a common skin concern that develops after inflammation, injury, or trauma to the skin.
It is caused by a number of skin conditions, including acne, dermatitis, burns, and melasma, as well as environmental factors such as UV damage.
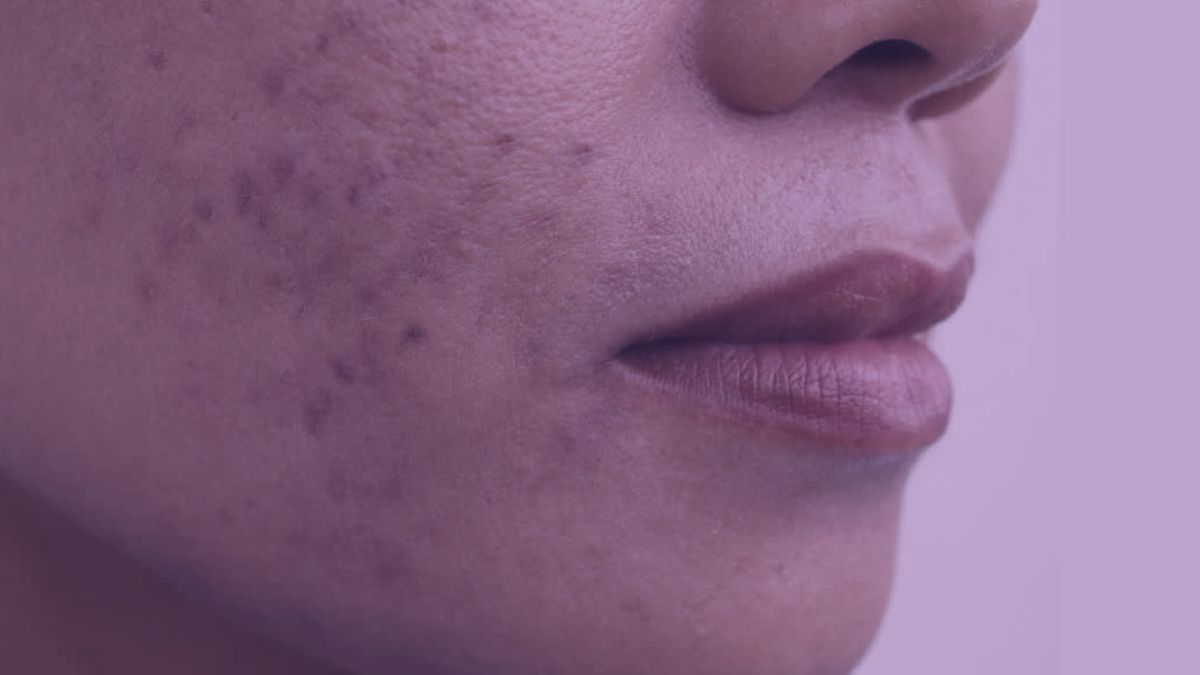
Post-inflammatory hyperpigmentation is characterized by dark spots or patches ranging in color from light brown to black and typically appears on the face, neck, chest, and other body areas.
However, while PIH can be stubborn and difficult to treat, with the potential to remain present for months and even years, many treatments can help reduce its appearance and even fully fade post-inflammatory hyperpigmentation.
Therefore, in this article, we will discuss the causes and symptoms of post-inflammatory hyperpigmentation, as well as various treatments available for it.
We will also discuss ways to prevent PIH from occurring in the first place and ensure the condition doesn’t worsen.
What Causes Post-Inflammatory Hyperpigmentation?
Here are some of the most common things that cause post-inflammatory hyperpigmentation:
• Acne: Acne is one of the most common causes of post-inflammatory hyperpigmentation, with dark spots or patches typically appearing after acne lesions have healed.
• Eczema: An inflammatory skin condition that flares up due to direct contact with an allergen or irritant; eczema can cause dark spots due to damage to the outer layers of skin, which can be made worse by itching.
• Psoriasis: Psoriasis is an autoimmune disorder that causes a buildup of skin cells, resulting in dry, itchy patches of red or purple scaly skin. These patches can cause PIH due to exposure to ultraviolet (UV) radiation from the sun.
• Allergic Reactions: Allergic reactions can be triggered by contact with substances such as latex, plants, and certain metals. This inflammation can lead to PIH in the affected area, especially if the reaction is severe or the skin has been itch-scratched.
• Skin Infections: Skin infections such as impetigo, bacterial folliculitis, and yeast infections can cause inflammation that can lead to PIH.
• Insect Bites: Insect bites can trigger an inflammatory reaction from the body, resulting in dark spots or patches.
• Incorrect Shaving: Incorrect shaving techniques can cause skin irritation and inflammation, leading to post-inflammatory hyperpigmentation, especially in areas where the hair is thick, such as the beard, bikini line, and legs.
• Friction or Pressure: Friction or pressure on the skin can cause dark spots, as can other skin injuries such as cuts and scrapes.
• Medication: Certain medications, such as antibiotics and steroids, can cause PIH by causing inflammation in the body and stimulating melanin production in the skin.
• Burns: Burns can lead to post-inflammatory hyperpigmentation when the burn heals and leaves a darker skin patch in its place.
Who Can Get Post-Inflammatory Hyperpigmentation?
Post-inflammatory hyperpigmentation can develop in all skin types, but it tends to be more pronounced and longer-lasting in people with dark skin, in whom the color tends to be more intense and persist for a more extended period than in lighter skin colors.
This is due to melanosomes, which are small pigmented organelles in the skin containing melanin, being larger and more abundant in dark skin tones, which means that when melanosomes are triggered, the flare is more prominent and takes longer to fade.
The Symptoms and Identification of PiH
Post-inflammatory hyperpigmentation may appear in various shapes and sizes, which usually indicates different causes.
Here are some of the most common symptoms of PIH and what might be causing it:
Dark Spots
The most common symptom of post-inflammatory hyperpigmentation is dark spots ranging in color from light brown to black and may be the same size or shape as the original injury.
These spots are usually the result of acne and appear in areas where the pimples used to be but have now healed. The spots may also appear in the same area as insect bites, rashes, razor burns, or other smaller skin injuries.
Dark Patches
Dark patches are larger, more spread out areas of discoloration that are the result of larger skin injuries such as burns, eczema, or a larger area of the body where there are folds or creases, such as the neck or armpits, due to conditions such as diabetes.
Uneven Skin Tone
Uneven skin tone is a slight darkening in larger areas of the face and body, which is usually the result of prolonged sun exposure and hormonal conditions such as melasma, which can cause the skin to become darker in certain areas due to hormonal imbalances, pregnancy, or medications that trigger excess production of the brown pigment responsible for our skin color.
Mechanism and Pathology of PiH
Post-inflammatory hyperpigmentation is a common skin condition characterized by darkening of the skin following an inflammatory event.
The underlying mechanism involves an increase in melanin production and its irregular distribution in the skin.
Melanin is the brown pigment mainly responsible for our skin color produced by cells called melanocytes. However, melanocytes are also a part of our skin’s immune system, as the melanin they produce helps protect against UV radiation and other environmental elements.
This is why melanocytes are super sensitive to inflammation, and when an inflammatory event occurs, they react strongly to it and increase the production of melanin because melanin is thought to neutralize reactive oxygen species, which, if not prevented, would cause further damage to the skin.
When this overproduction occurs due to inflammation, it leads to clumps or an uneven distribution of the pigment in the skin cells within the skin layers.
This results in the affected skin cells becoming darker than the surrounding, healthy skin cells, leading to what we see as hyperpigmentation, discoloration, or uneven skin tone on the surface.
Risk Factors That Increase the Chances of Post-Inflammatory Hyperpigmentation
Here are several factors that may increase the risk of post-inflammatory hyperpigmentation:
• Genetic Predisposition: Acne and hyperpigmentation can be hereditary, meaning that if your parents have it, you may be more likely to develop it too.
• Dark Skin: People with darker skin tones are more prone to PIH due to the more abundant presence of melanosomes in their skin.
• Working Outdoors: Excess sun exposure for prolonged periods can trigger PIH as the UV rays cause skin inflammation and attack vital parts of the skin cells’ DNA that control their pigmentation.
• Working With Hazardous Chemicals: Working with chemicals, such as those found in some industrial settings or beauty salons, can increase the risk of developing PIH due to potential burns and injuries these chemicals can cause when in contact with our skin.
• Working With Sharp Objects or Machinery: Working with sharp objects or machinery can easily cause minor injuries and skin irritations that may lead to PIH.
• Medications: Some steroids, antibiotics, and even birth control pills can sometimes cause hyperpigmentation as a side effect.
• Poor Skincare: Incorrect usage of skincare products, such as harsh ingredients or over-exfoliation, can lead to skin inflammation and increased risk of PIH.
• Age: Skin becomes more vulnerable to inflammation and subsequent hyperpigmentation as we age due to natural aging processes that weaken our skin’s protective barrier and make it more susceptible to environmental damage.
What Can Make Post-Inflammatory Hyperpigmentation Worse?
Sun exposure is one of the most common factors that can worsen the appearance of post-inflammatory hyperpigmentation.
The UV rays will darken the affected patches as the sun is also closely associated with other forms of hyperpigmentation, such as age spots.
This will also prolong the healing time.
How to Treat Post-Inflammatory Hyperpigmentation?
Post-inflammatory hyperpigmentation is a stubborn skin condition that can stick around for a long time if not addressed adequately and in time.
Therefore, here are some fantastic ways to help fade existing hyperpigmentation and prevent it from forming in the future:
Diet Changes
When trying to improve your chances of fading post-inflammatory hyperpigmentation, reducing sugar or completely cutting it out of your diet is one of the things you should consider doing.
Sugar is a highly inflammatory component high on the glycemic index, which means it creates inflammation in the body.
This inflammation can sometimes manifest on the skin in the form of inflammatory skin conditions such as acne, which can then lead to post-inflammatory hyperpigmentation.
Additionally, sugar can lead to hormonal imbalances, which can trigger skin conditions such as melasma, a discoloration that’s difficult to treat and notorious for returning.
Finally, excessive sugar consumption can also lead to life-threatening conditions such as diabetes, which can also manifest on your skin as discoloration and darkening in certain areas that have folds or creases, such as the neck and armpits.
Therefore, reducing or eliminating sugar from your diet can be a great way to help reduce the risk of developing post-inflammatory hyperpigmentation and fade existing discoloration.
Lifestyle Changes
Making lifestyle changes to reduce stress, get better sleep, and create healthier habits can also help in the long run when it comes to fading post-inflammatory hyperpigmentation.
Stress is known to increase inflammation in the body and lead to skin conditions such as acne that can leave discoloration once they clear up.
Similarly, avoiding excessive alcohol consumption and quitting smoking can also help prevent hyperpigmentation from forming on your skin, as these habits are known to worsen discoloration by dehydrating the skin and harming vital parts of our skin cells.
Additionally, getting enough sleep and following a healthy diet can help reduce the risk of skin conditions that can lead to PIH.
Finally, limiting sun exposure and wearing protective gear when working with chemicals and machinery that could cause some sort of skin trauma can also help in reducing the risk of developing post-inflammatory hyperpigmentation in the long run.
Skincare Products
Besides wearing sunscreen to ensure there’s a barrier between your skin and one of the main factors that can exacerbate post-inflammatory hyperpigmentation (UV rays), you also need to incorporate components known as melanin inhibitors into your skincare routine.
These ingredients can stop the process responsible for excess melanin production by inhibiting the enzyme tyrosinase, which directly triggers the melanocytes responsible for melanin production.
Here are some of the best products and melanin-inhibiting components to incorporate into your skincare routine when treating PIH:
• Retinoids: These are vitamin A derivatives that boost cellular turnover, which helps remove layers of skin discoloration and stimulates collagen production for a more even-toned complexion.
• Alpha Hydroxy Acids (AHAs): These exfoliating acids help fade uneven skin tone, dark spots, and discoloration by dissolving the glue that holds pigmented dead skin cells on the skin’s surface together and encouraging them to shed naturally.
• Kojic Acid: Kojic acid is a natural ingredient derived from mushrooms that act as a melanin inhibitor, and it helps fade discoloration by preventing the formation of new pigmentation.
• Tranexamic Acid: This component has been proven to effectively reduce pigmentation by preventing the absorption of UV rays and inhibiting melanogenesis.
• Alpha Arbutin: This extract from dried plant leaves such as blueberry, cranberry, and bearberry helps reduce existing pigmentation and prevent new spots from forming.
• Vitamin C: A potent antioxidant that reduces free radical activity in the skin and repairs cell DNA damage caused by environmental factors such as UV rays and pollution.
• Niacinamide: Also known as vitamin B3, niacinamide can help brighten skin tone by blocking the transfer of melanin to the surface and increasing ceramide production.
The best skincare products to tackle post-inflammatory hyperpigmentation are serums.
This is because they are lightweight, and they’re usually packed with multiple brightening actives.
The Best Serums for Post-Inflammatory Hyperpigmentation
Here are six fantastic serums for post-inflammatory hyperpigmentation you can incorporate into your skincare routine to fade discoloration and even out your skin tone:
Paula’s Choice 20 Niacinamide Treatment

• Best for mild hyperpigmentation.
The 20 Niacinamide Treatment by Paula’s Choice is a powerhouse of concentration that helps improve the texture and tone of your skin.
This serum is formulated with 20% niacinamide, which helps reduce acne, inflammation, and redness, minimizes the appearance of enlarged pores, fades mild to moderate hyperpigmentation, corrects discolored areas, and boosts the skin’s natural barrier function.
It also contains brightening antioxidants such as vitamin C and redness-reducing green tea extract to help protect the skin from environmental stressors.
Paula’s Choice CLINICAL 1 Retinol Treatment

Best for experienced retinol users.
The Paula’s Choice, 1% Retinol Serum from the CLINICAL line, is a lightweight, creamy serum with the highest percentage of retinol you can get over the counter.
The retinol in this formula is encapsulated, which means it will refine pore size, diminish the appearance of wrinkles, fine lines, uneven skin tone, and even more stubborn hyperpigmentation.
However, it will be released into the skin over time to prevent irritation and excessive shedding.
Besides that, the formula contains nourishing licorice and oat extracts along with other soothing plant extracts to calm and soothe the skin and hyaluronic acid to keep it hydrated.
The 1% Retinol Serum is an excellent product if you want to bump up your retinol’s strength and tackle mild to moderate PIH.
Vivant Skin Care 15% Mandelic Acid Serum

Best for acne scarring.
Vivant’s 15% Mandelic Acid Serum is an exfoliating serum containing a blend of mandelic and lactic acid – two AHAs that lift dead skin cells, unclog pores, soothe inflammation, reduce acne, and hydrate the skin.
Besides that, this serum also contains urea, an organic compound with hydrating properties that works well in combination with AHAs, niacinamide, and inositol, both parts of the vitamin B family known for their anti-inflammatory and brightening properties.
Last but not least, the serum also contains Sodium PCA, which is one of the skin’s natural moisturizing factors.
Lightweight, gentle, and excellent for acne-prone skin and subsequent scarring, this serum leaves a mild glow on the skin and is perfect for those just getting into acids.
SkinCeuticals Discoloration Defense

Best for uneven skin tone.
SkinCeuticals Discoloration Defense is a gentle brightening serum formulated with niacinamide, tranexamic acid, kojic acid, and 5% HEPES, a synthetically-derived acid that dissolves the bonds binding dead skin cells together and encourages them to shed.
Fantastic for anyone with sensitive skin who doesn’t want to include more aggressive treatments such as retinoids and exfoliating acids in their skincare routine, this serum can help reduce the appearance of post-inflammatory hyperpigmentation, discoloration and uneven skin tone.
iS Clinical Active Serum

Best for anti-aging.
iS CLINICAL’s Active Serum is a lightweight serum that feels like water on the skin but is packed with active ingredients that target multiple skin concerns and conditions.
There is quite an assortment here, starting with arbutin and mushroom extract, which minimize the appearance of uneven skin tone and brighten post-inflammatory hyperpigmentation.
Moving forward, the serum contains white willow bark extract, which is essentially salicylic acid that deeply cleanses the pores and dissolves all the gunk inside there that’s causing acne breakouts.
Additionally, the serum also contains sugar cane extract derived from the tropical grass sugarcane, a natural exfoliant and a humectant that helps the skin attract and retain moisture.
And lastly, there is Bilberry extract, which is one of the best sources of antioxidant compounds that help strengthen the skin, even out the skin tone, and soothe redness due to their calming properties.
Although super pricey, the Active Serum is worth the splurge and can be used on almost all skin types, but it is perfect for those with coarse, oily, and acne-prone skin with mild to moderate PIH and signs of skin aging.
SkinCeuticals C E Ferulic

Best for sun damage.
A gold standard in the treatment of sun-damaged skin, discoloration, and post-inflammatory hyperpigmentation, the SkinCeuticals C E Ferulic is an antioxidant serum that boasts a combination of ferulic acid, a potent antioxidant that stabilizes vitamin C, along with pure vitamin C and healing vitamin E to enhance the skin’s protection against environmental damage caused by free radicals in the air.
In addition to antioxidant protective benefits, this formula improves signs of aging and photodamage to reduce the appearance of lines and wrinkles while firming and brightening your complexion.
Lastly, this powerful formula helps neutralize free radicals induced by UVA/UVB, infrared radiation (IRA), and ozone pollution (O3).
Ready to take control of your skincare journey and conquer acne-related issues like Post-Inflammatory Hyperpigmentation (PIH)?
Discover the ultimate solution with my comprehensive course, “The Acne Solution.”
This course is meticulously designed to empower you with the knowledge and tools needed to achieve clear, radiant skin.
Enroll today and enjoy benefits such as:
- In-depth understanding of acne causes and triggers.
- Proven strategies to effectively manage PIH and prevent future occurrences.
- Personalized skincare routines tailored to your unique skin type and concerns.
- Access to expert guidance, tips, and insider secrets for flawless skin.
Don’t let acne hold you back any longer.

My name is Simone and I am a certified skin specialist. I created this website to teach my readers how to take great care of their skin and I also like to occasionally share my honest opinions on skincare products I’ve tried. You can learn more about me here.
